That sharp, stabbing pain when you take your first steps out of bed in the morning – most people brush it off as stiffness. But if it keeps coming back day after day, it has a name: plantar fasciitis. And for many patients, it comes with an unwanted companion – a heel bone spur (also called a calcaneal spur).
This guide is written for anyone dealing with persistent heel pain, whether you’re a teacher who stands all day, a runner, or someone who simply cannot figure out why the bottom of their heel hurts. We’ll break down the anatomy, the causes, and – most importantly – what you can actually do about it.
Table of Contents
What is Plantar Fasciitis?

Plantar fasciitis (pronounced “plan-ter fash-ee-EYE-tis”) is one of the most common causes of heel pain. It affects millions of people globally and accounts for a significant portion of all foot-related orthopaedic visits.
The plantar fascia is a thick band of connective tissue – almost like a bowstring – that runs along the bottom (plantar surface) of your foot. It connects your heel bone (calcaneus) to your toes and plays a critical role in supporting your foot’s arch during walking, running, and standing.
When this tissue gets overstressed, it develops tiny micro-tears. Your body responds with inflammation. Inflammation is what causes the characteristic pain in the heel of the foot, especially at the bottom of the heel and along the arch.
Why Does Plantar Fasciitis Hurt Most in the Morning?
This is one of the most frequently asked questions – and the answer is rooted in biology.
When you sleep, your plantar fascia contracts and tightens overnight. The moment you put weight on it with your first steps, those tight, inflamed fibres are suddenly stretched and stressed. The result: that signature sharp, stabbing pain in the heel of the foot in the morning.
After a few minutes of walking, the tissue warms up and loosens, which is why the pain often fades – only to return after long periods of sitting or standing.
What is a Heel Bone Spur (Calcaneal Spur)?

A heel spur – medically called a calcaneal spur or plantar calcaneal spur – is a bony projection that grows on the underside or back of the heel bone (calcaneus). It forms slowly over months or years as the body deposits calcium in response to repeated stress or tension at the attachment point of the plantar fascia.
On an X-ray (heel spur X-ray), it appears as a small hook or point jutting out from the calcaneus, which is why it’s sometimes described as a bone growth on the foot or bone enlargement in the heel.
Are Heel Spurs and Plantar Fasciitis the Same Thing?
No – but they are closely related. This is a source of significant confusion.
- Plantar fasciitis = inflammation of the plantar fascia tissue
- Calcaneal spur = a bony growth that forms at the heel
Many patients with plantar fasciitis also have a calcaneal spur on X-ray. However, the spur itself is usually not the cause of the pain – the inflamed fascia is. In fact, studies show that many people with visible heel spurs on imaging experience no pain at all.
Think of it this way: the spur is a byproduct of chronic stress on the heel, not the villain.
Who Gets Plantar Fasciitis? Common Causes and Risk Factors

Plantar fasciitis doesn’t discriminate – it affects athletes and desk workers alike. But certain factors make you significantly more likely to develop it.
Most Common Causes of Plantar Fasciitis:
- Overuse and repetitive strain – Running, jumping, or standing for extended periods puts repeated micro-stress on the plantar fascia
- Flat feet (pes planus) – Flat foot plantar fasciitis is common because poor arch support increases tension along the fascia
- High arches – Paradoxically, very high arches also create abnormal load distribution
- Tight calf muscles or Achilles tendon – A tight Achilles tendon is one of the strongest predictors of plantar fasciitis, since tension travels directly into the heel
- Sudden increase in activity – Starting a new exercise program too aggressively
- Improper footwear – Worn-out shoes with inadequate arch support or walking barefoot on hard surfaces
- Obesity or sudden weight gain – Excess body weight dramatically increases the mechanical load on the heel
- Age – Most common in people between 40 and 60 years, as tissue elasticity decreases
- Occupational factors – Teachers, nurses, factory workers, and retail staff who stand on hard floors all day
What Causes Heel Spurs Specifically?
Calcaneal spur causes overlap heavily with plantar fasciitis triggers. The sustained pulling of the plantar fascia at its insertion into the calcaneus triggers calcium deposition over time. This is essentially the body trying to reinforce a chronically stressed attachment site – which is why heel spurs and plantar fasciitis so frequently coexist.
Recognising the Symptoms: Is This Plantar Fasciitis?
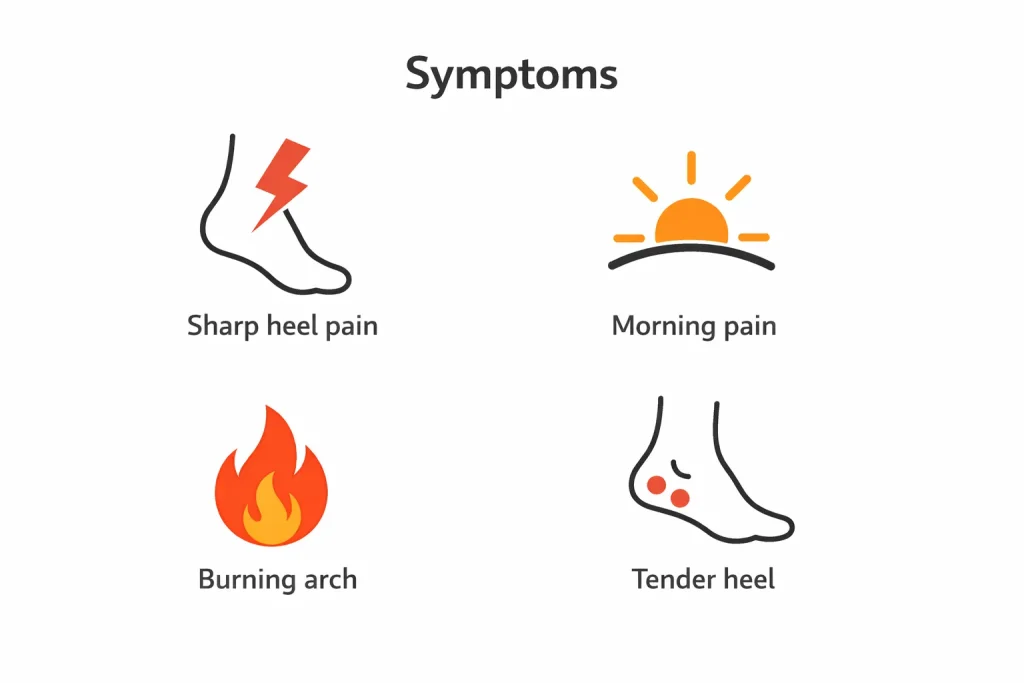
Classic Plantar Fasciitis Symptoms:
- Sharp, stabbing pain at the bottom of the heel – especially with the first steps in the morning or after prolonged rest
- Pain that improves with movement but returns after long periods of standing or walking
- Aching or burning sensation along the arch of the foot
- Tenderness when pressing on the inner heel – a hallmark sign used during clinical examination
- Increased pain after (not during) exercise – unlike many injuries, it tends to flare up post-activity
- Stiffness and tightness along the plantar surface of the foot
Calcaneal Spur Symptoms:
Interestingly, most heel spurs (calcaneal spur symptoms) are asymptomatic. When symptoms do occur, they typically mirror plantar fasciitis: pain in the heel pad, pain on the sole of the heel, and discomfort with prolonged standing or walking.
When Should You Be Concerned?
Seek medical attention if:
- Pain has persisted for more than 4–6 weeks without improvement
- You have significant heel swelling or bruising
- Pain is severe enough to limit normal daily activities
- You’ve tried conservative measures and see no progress
- You experience numbness or tingling in the heel or foot (may indicate nerve involvement)
Diagnosis: How Doctors Confirm Plantar Fasciitis and Heel Spurs

A diagnosis of plantar fasciitis is primarily clinical – meaning your doctor can often diagnose it through a careful history and physical examination alone.
What to expect at your appointment:
- Medical history – Duration, location, and pattern of pain; activities; footwear; previous injuries
- Physical examination – Palpation of the heel, assessment of foot arch, Achilles tendon tightness, and range of motion
- X-ray (heel pain X-ray) – Helps identify a calcaneal spur, rules out fractures or other bony pathology. A plantar calcaneal spur on X-ray appears as a bony projection at the heel’s inferior border
- Ultrasound – Can directly visualise plantar fascia thickening and inflammation with high accuracy
- MRI – Used in complex or resistant cases; plantar fasciitis radiology via MRI shows oedema and thickening of the fascial band
It is important to note that bilateral plantar fasciitis (affecting both feet simultaneously) is less common and may warrant further investigation to rule out systemic or inflammatory conditions.
Treatment: A Step-by-Step Approach

The good news is that over 90% of plantar fasciitis cases resolve with conservative, non-surgical treatment – though it requires patience and consistency. Here is a structured approach from conservative to advanced.
Stage 1 – Initial Relief (Weeks 1–4)
Rest and Activity Modification
This doesn’t mean complete bed rest – it means reducing the activities that aggravate your heel. Swap high-impact activities like running for swimming or cycling during the acute phase.
Ice Therapy
Apply an ice pack wrapped in a cloth to the heel for 15–20 minutes, 3–4 times per day – especially after activity. Rolling a frozen water bottle under the foot serves double duty: cold therapy + gentle massage.
Anti-Inflammatory Medications
Over-the-counter NSAIDs (like ibuprofen) can help manage plantar fasciitis inflammation and pain in the short term. Always consult your doctor before starting any medication.
Footwear Assessment
- Switch to supportive footwear for heel pain with adequate arch support and cushioning
- Avoid walking barefoot on hard floors
- Consider heel cushions for plantar fasciitis or heel cups – these orthopedic heel pain products redistribute load away from the inflamed area
- Footwear for heel spurs should have a slight heel raise and a firm midsole
Stage 2 – Stretching and Rehabilitation (Weeks 2–8)
This is where real recovery happens. Consistent stretching is the most evidence-backed conservative treatment for plantar fasciitis.
Essential Calcaneal Spur Exercises and Plantar Fasciitis Stretches:

1. Plantar Fascia Stretch (Towel/Band Stretch)
- Sit on a chair, cross one foot over the opposite knee
- Pull your toes back gently toward your shin using your hand or a towel
- Hold for 30 seconds, repeat 3 times per session
- Do this before your first step in the morning – it dramatically reduces morning pain
2. Calf Stretch Against the Wall
- Stand facing a wall, step one foot back
- Keep the back knee straight and press the heel firmly into the floor
- Hold for 30 seconds, 3 repetitions each side
- A tight calf directly increases plantar fascia tension – this stretch is essential
3. Towel Toe Curls
- Place a small towel on the floor and scrunch it toward you using only your toes
- Strengthens the intrinsic foot muscles that support the arch
4. Marble Pick-Up
- Place marbles on the floor and pick them up with your toes
- Improves plantar fascia flexibility and foot strength
5. Frozen Bottle Roll
- Roll the arch of your foot over a frozen water bottle for 5–10 minutes
- Combines massage with ice therapy – excellent for acute flare-ups
6. Seated Towel Stretch
- Loop a towel around the ball of your foot while seated
- Gently pull toward you to stretch the plantar fascia
- 3 sets of 30 seconds, morning and evening
Key insight: Consistency matters more than intensity. Doing these plantar fasciitis exercises daily – even when pain subsides – prevents relapse. Most patients who stop stretching once pain fades see symptoms return within weeks.
Stage 3 – Orthotic Support and Taping
Custom or Prefabricated Orthotics
Orthotics fit inside your shoes and correct biomechanical issues like flat feet or abnormal pronation that contribute to plantar fasciitis. They provide plantar heel support and distribute ground reaction forces more evenly across the foot.
Taping for Calcaneal Spur and Plantar Fasciitis
Low-Dye or Kinesiology taping temporarily supports the plantar fascia and reduces load on the inflamed tissue. This is particularly useful for people who must stay on their feet for work.
Night Splints
Night splints hold the foot in a dorsiflexed (toes-up) position while you sleep – keeping the plantar fascia gently stretched overnight. This is one of the most effective ways to eliminate morning pain, with studies showing significant improvement in a majority of patients.
Stage 4 – Physiotherapy and Advanced Conservative Care
A qualified physiotherapist can provide:
- Manual therapy – Soft tissue mobilisation, joint manipulation
- Ultrasound therapy – Promotes healing in the plantar fascia
- Shockwave therapy (ESWT) – Extracorporeal shockwave therapy has strong evidence for chronic plantar fasciitis that hasn’t responded to 3–6 months of conservative care. Delivers high-energy sound waves to the heel to stimulate healing
- Calcaneal spur physiotherapy – Targeted programs combining stretching, strengthening, and load management
- Gait analysis – Identifies walking or running patterns contributing to overload
Stage 5 – Injections
Corticosteroid Injection (Calcaneal Spur Injection)
A steroid injection into the plantar fascia can provide significant short-term pain relief when conservative measures fall short. However, repeated injections are discouraged as they can weaken the plantar fascia and increase rupture risk.
Platelet-Rich Plasma (PRP) Injection
An emerging treatment where the patient’s own blood is processed and injected into the heel. PRP shows promise for chronic plantar fasciitis cases unresponsive to other treatments.
Stage 6 – Surgery (Last Resort)
Heel spur surgery and plantar fascia release are considered only after 6–12 months of failed conservative treatment, affecting fewer than 5% of patients.
Plantar Fascia Release involves surgically cutting part of the plantar fascia to relieve tension. Heel spur removal (calcaneal spur surgery) may be performed simultaneously, though evidence suggests the spur is rarely the pain generator.
Calcaneal spur surgery recovery time typically ranges from 6–10 weeks, with full return to activity by 3–6 months. It is an effective but serious intervention with real risks, including infection, nerve damage, and arch collapse.
What to Wear: Footwear and Heel Pain Products
Shoe choice has an outsized impact on plantar fasciitis recovery and prevention.
What to look for in footwear for heel pain:
- Firm, well-cushioned midsole
- Adequate arch support (not flat insoles)
- Slight heel raise (10–15mm) reduces plantar fascia tension
- Wide toe box to prevent forefoot compression
- Replace running shoes every 500–700 km – worn-out cushioning is a common trigger
Heel pain products that help:
- Gel heel cups or heel pain caps – Absorb shock at the point of impact
- Plantar fasciitis heel cushions – Provide targeted support under the arch
- Orthopedic shoes for heel pain – Specially designed footwear with built-in support features
- Night splints – For morning pain relief
Avoid: flat flip-flops, worn-out sneakers, and prolonged barefoot walking on hard floors.
Unique Insight: Why Most Patients Recover – And Why Some Don’t
The patients who recover fully from plantar fasciitis typically have two things in common: they stretch consistently, and they address the underlying cause (footwear, biomechanics, activity load).
The patients who struggle tend to:
- Stop treatment as soon as pain eases (before the fascia has healed)
- Return to high-impact activity too quickly
- Ignore footwear issues
- Delay seeking care until the condition has become chronic (more than 6 months)
Chronic heel pain is significantly harder to treat than early-stage plantar fasciitis. The message is simple: start treatment early, be consistent, and don’t self-diagnose as “just sore.”
Plantar Fasciitis vs Heel Spur: A Clear Comparison
| Feature | Plantar Fasciitis | Heel Spur (Calcaneal Spur) |
| What it is | Inflammation of the plantar fascia | Chronic tension at the fascia insertion |
| Cause | Repetitive stress, overuse | Chronic tension at fascia insertion |
| Visible on X-ray | No (soft tissue) | Yes – bony projection on calcaneus |
| Always painful | Yes (when active) | Not necessarily |
| Treated by | Stretching, physio, orthotics | Same as plantar fasciitis; rarely surgery |
| Relationship | Often coexist | Develops as a result of fasciitis |
Conclusion and Actionable Takeaways
Heel pain from plantar fasciitis and bone spurs is extremely common – but it is also very treatable. The vast majority of patients recover fully without surgery, provided they take a structured, consistent approach.
Your action plan:
- Start stretching immediately – morning plantar fascia stretch before your first step is non-negotiable
- Assess your footwear and invest in supportive shoes or orthotic insoles
- Apply ice after activity to manage inflammation
- See an orthopaedic specialist if pain persists beyond 4–6 weeks
- Ask about shockwave therapy if you’ve had symptoms for several months
- Do not ignore bilateral heel pain – get it properly evaluated
The single most important thing: don’t wait. Early intervention leads to faster recovery and prevents plantar fasciitis from becoming a chronic, debilitating condition.
Frequently Asked Questions
What is the fastest way to cure plantar fasciitis?
There is no single overnight cure, but the fastest recovery comes from combining daily plantar fascia stretching, ice therapy, supportive footwear, and rest from high-impact activities. Patients who follow this consistently often see significant improvement within 4–6 weeks.
Can plantar fasciitis go away on its own without treatment?
In mild cases, symptoms may ease with rest alone – but without addressing the underlying causes (tight calves, poor footwear, biomechanics), plantar fasciitis typically recurs. Structured treatment prevents it from becoming chronic.
Is a heel bone spur the same as plantar fasciitis?
No. Plantar fasciitis is inflammation of the plantar fascia tissue, while a calcaneal spur is a bony calcium deposit on the heel bone. They often coexist, but the spur itself is frequently not the source of pain – the inflamed fascia is.
How do I know if I have a heel spur?
A heel spur (calcaneal spur) can only be definitively identified on an X-ray of the heel. Clinically, it may present with pain at the bottom of the heel, but many heel spurs are discovered incidentally during imaging for plantar fasciitis.
What exercises help plantar fasciitis and calcaneal spurs?
The most effective exercises include the plantar fascia towel stretch (pulling toes back), calf stretches against a wall, frozen bottle rolling, and towel toe curls. These should be done daily, especially first thing in the morning and after periods of rest.
When should I see a doctor for heel pain?
See an orthopaedic specialist if your heel pain has lasted more than 4–6 weeks, is severe enough to affect daily activities, is associated with swelling or numbness, or has not improved with rest and home treatment. Early intervention leads to better outcomes.