You bent down to pick something up – nothing dramatic, nothing heavy – and suddenly your lower back screamed. Or maybe the pain crept in slowly over weeks, starting as a dull ache and growing into a sharp, shooting sensation that travels down your leg. Either way, you are now wondering: Is this a herniated disk?
If so, you are not alone. Lower back pain is one of the most common health complaints in the world, and a herniated disk in the lower back is one of its leading causes. The good news is that the vast majority of people recover without surgery – and there is quite a bit you can do on your own to manage pain, speed up healing, and get your life back.
This guide covers everything you need to know: what a herniated disk actually is, why it happens, the symptoms to watch for, and the practical self-care steps you can take starting today.
Table of Contents
What is a Herniated Disk in the Lower Back?
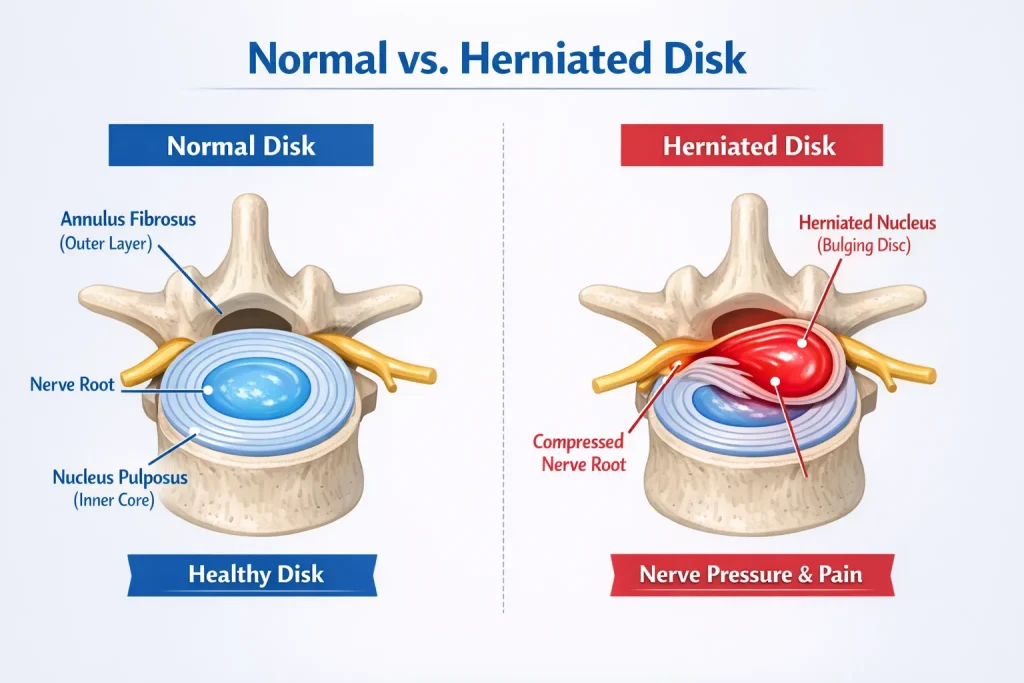
Your spine is a column of 24 stacked bones called vertebrae. Between each pair of vertebrae sits a small cushion-like structure called an intervertebral disk. These disks absorb shock every time you walk, run, or simply sit down at a desk.
Each disk has two layers:
- The outer layer is a tough, fibrous ring called the annulus fibrosus
- The inner layer is a soft, gel-like substance called the nucleus pulposus
When everything is working normally, that gel stays neatly inside the ring. A herniated disk – sometimes called a ruptured or slipped disk – happens when that gel pushes outward through the outer ring and presses on the surrounding nerves.
Most herniations happen in the lumbar spine, which is the lower part of your back made up of five vertebrae. That is because the lumbar spine bears most of your body weight and is involved in almost every movement you make.
The Anatomy Behind the Pain
Understanding why a herniated disk hurts so much comes down to one word: nerves. Your spinal cord runs through a channel inside your vertebrae, and nerve roots branch off from it at every level.
When a herniated disk bulges outward, two things happen at the same time:
- The disk physically compresses the nearby nerve root
- The gel material inside the disk releases inflammatory chemicals that irritate the nerve tissue
You are getting a double hit – mechanical pressure and chemical inflammation at the same time. That is why herniated disk pain can be so intense and persistent.
What Causes a Herniated Disk?
There is rarely a single dramatic moment that causes a herniated disk. For most people, it is the cumulative result of years of stress on the spine combined with the natural aging process.
Age and Disk Degeneration
Disk degeneration is a normal part of getting older. Here is what happens over time:
- In youth, spinal disks are plump and hydrated – roughly 80% water
- As you age, they gradually dry out and lose elasticity
- The outer ring becomes more brittle, and the spaces between vertebrae narrow
- By your 30s or 40s, a minor movement – a sneeze, an awkward twist, leaning forward too quickly – can be enough to cause a herniation
This process of disk degeneration is normal and inevitable to some degree, but how fast it happens is heavily influenced by your daily habits.
Lifestyle and Daily Habits That Put Your Spine at Risk
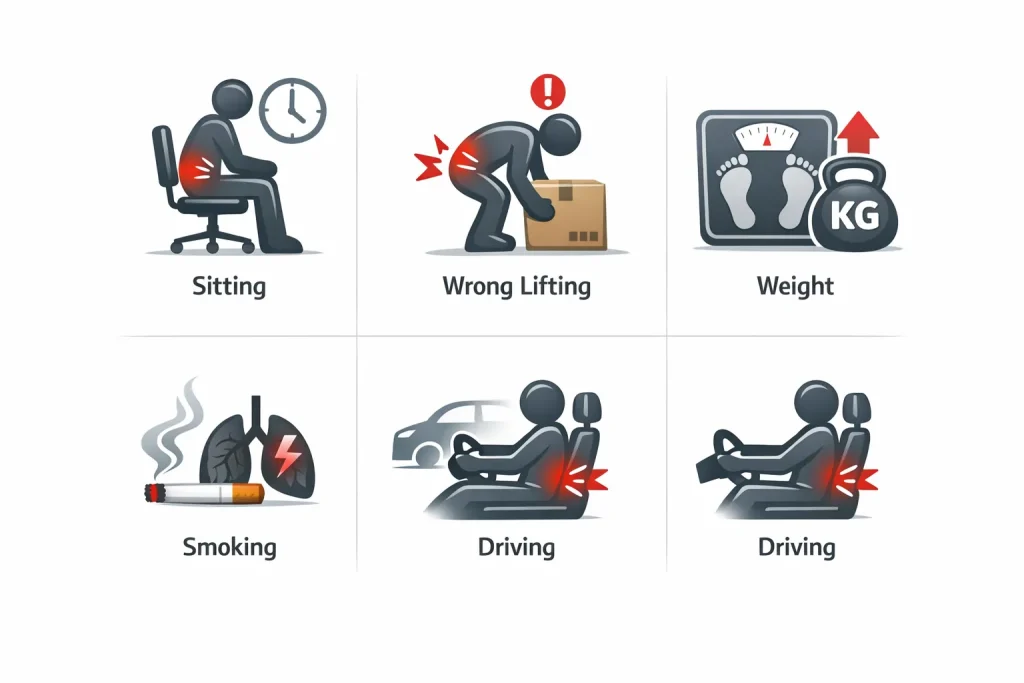
Several everyday habits quietly accelerate disk breakdown and raise your risk of herniation:
- Lifting with your back instead of your legs. When you hinge forward at the waist to pick something up, your lower back muscles work against enormous leverage. Over time, or with one heavy enough load, this can force the gel nucleus through the outer wall of the disk.
- Prolonged sitting. Sitting – especially with poor posture – puts more pressure on your lumbar disks than standing does. People who spend most of their day seated, whether at a desk or behind a wheel, are putting their lower back under constant low-grade stress.
- Excess body weight. Extra weight, particularly around the midsection, shifts your center of gravity forward and adds sustained pressure to the lumbar spine. Over the years, this has accelerated disk wear significantly.
- Sedentary lifestyle. The muscles of your core – your abdominals, obliques, and lower back muscles – are what stabilize your spine. When those muscles are weak from inactivity, your disks have to compensate for forces they were not designed to handle alone.
- Smoking. Smoking restricts blood flow and reduces oxygen delivery to spinal disks, which speeds up degeneration. If you smoke and have back pain, quitting is one of the most meaningful things you can do for your spine.
- Repetitive strain at work. Jobs that involve constant bending, twisting, lifting, or pulling create repeated micro-stress on the lumbar disks. Using proper body mechanics consistently – not just when you remember – is essential in physically demanding roles.
- Frequent driving. Staying seated for long periods combined with engine vibration puts pressure on your spine and disks over time.
Worth knowing: Men between the ages of 20 and 50 are statistically the most likely group to develop a herniated disk in the lower back. However, sedentary desk workers of any age and gender are increasingly at risk due to the postural demands of modern work life.
Symptoms You Should Not Ignore
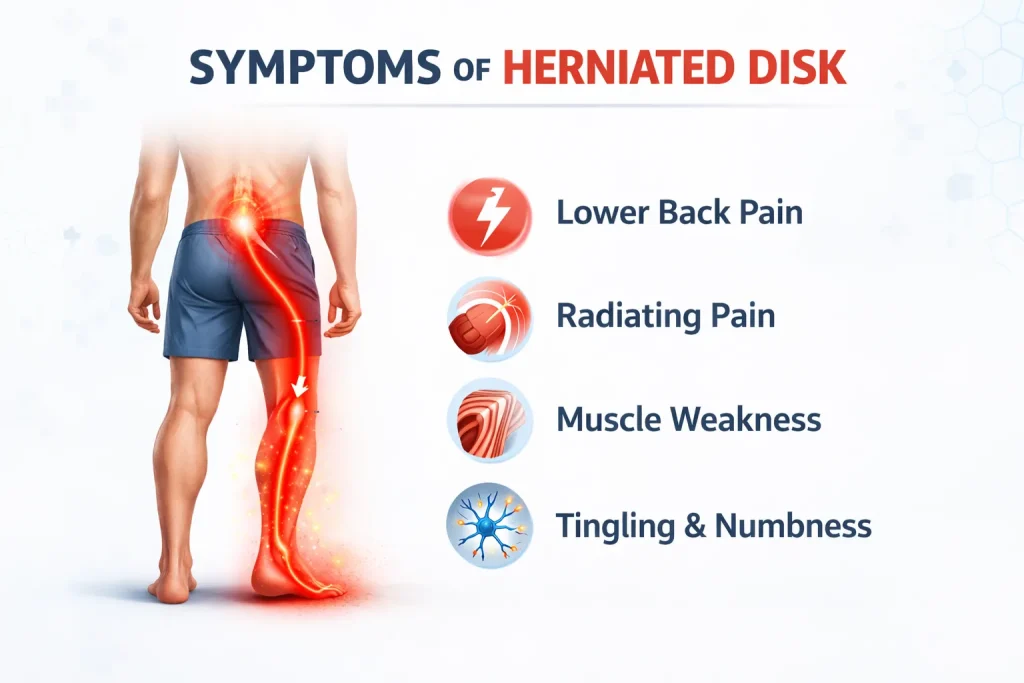
Herniated disk symptoms vary widely depending on exactly which disk is affected and how much pressure is placed on the surrounding nerves. Some people have a herniated disk and feel nothing at all. Others experience symptoms that stop them completely.
The most common first symptom is lower back pain that comes on suddenly or builds gradually over days. This pain can range from a dull aching to sharp, stabbing pain that worsens with movement, coughing, or sneezing.
Other common symptoms include:
- A shooting or burning pain that travels from the lower back down through the buttock and leg (sciatica)
- Numbness or tingling sensation in the leg and foot
- Weakness in the leg or foot – your foot may not lift as easily as usual
- Pain that is worse when sitting and slightly better when walking or lying down
Sciatica – The Classic Warning Sign
When a herniated disk presses on the sciatic nerve – the large nerve that runs from your lower back through your buttocks and down each leg – you experience what is known as sciatica.
Sciatica feels like:
- An electric shock traveling down the leg
- A burning or shooting pain from the buttocks into the thigh and calf
- Pins and needles or numbness in the lower leg or foot
- Muscle weakness on the affected side
It usually affects only one side of the body. Sciatica is one of the clearest signs that a herniated lumbar disk is pressing on a nerve root.
When Lower Back Pain Becomes an Emergency
One symptom combination should prompt you to seek medical care immediately without waiting – loss of bladder or bowel control. This is a rare but serious condition called cauda equina syndrome, where the nerve roots at the base of the spinal cord are severely compressed.
If you experience loss of bladder or bowel control alongside back and leg pain, go to an emergency room right away. Do not try to manage this at home.
Self-Care Steps You Can Take at Home
Here is the reassuring reality: roughly 90% of herniated disk cases get better without surgery. The disk material often naturally shrinks and gets reabsorbed by the body over time. Your job during that healing window is to manage your pain, protect your spine from further stress, and gradually rebuild the strength that supports recovery.
Rest the Right Way
When pain flares, your instinct might be to lie down and stay down. A day or two of rest is reasonable and can relieve significant pressure on the affected nerves. However, extended bed rest slows recovery.
Here is how to rest smartly:
- Limit bed rest to one to two days maximum during a flare-up
- Avoid sitting for more than 30 to 45 minutes at a stretch without a short walk
- Move slowly and in a controlled way when you do get up – no sudden movements
- Avoid bending forward at the waist, heavy lifting, or twisting your trunk
- Lie on your back with a pillow under your knees – this is often the most comfortable position for lumbar disk pain
Use Heat and Ice Strategically
Both heat and cold can be valuable tools for managing pain at home. The trick is knowing when to use which.
- In the first 24 to 72 hours: Use ice. Apply a cold pack wrapped in a cloth to your lower back for 15 to 20 minutes at a time, several times a day. Cold reduces inflammation and numbs the area.
- After the initial phase: Switch to heat. A warm heating pad or hot water bottle relaxes tight muscles, improves circulation, and makes gentle movement much easier.
- Never apply heat or ice directly to bare skin
- Never sleep with a heating pad in place
Over-the-Counter Pain Relief
Nonsteroidal anti-inflammatory drugs – NSAIDs like ibuprofen and naproxen – are commonly recommended for herniated disk pain. They work on two levels:
- They reduce inflammation around the irritated nerve root
- They provide general pain relief that makes it easier to stay mobile
Take them as directed and with food to protect your stomach. If NSAIDs are not suitable for you due to stomach, kidney, or heart conditions, acetaminophen provides pain relief as an alternative, though it does not address inflammation directly. Always check with your doctor if you are unsure.
Gentle Exercises and Stretches
Movement is medicine for a herniated disk – but the wrong movements at the wrong time can make things worse. In the early stages, the goal is to gently restore mobility and relieve nerve pressure, not aggressively strengthen.
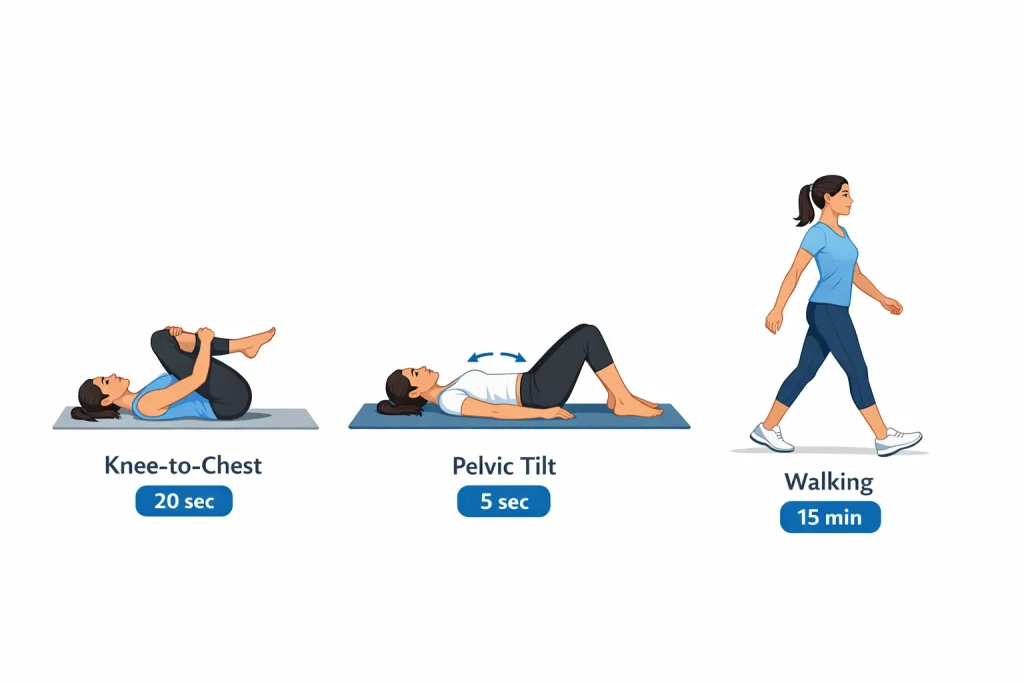
Movements that many people with lumbar disk herniation find helpful:
- Knee-to-chest stretch. Lie on your back with knees bent. Slowly bring one knee toward your chest and hold with both hands for 20 to 30 seconds. Repeat with the other leg. This gently stretches the lower back and releases the piriformis muscle, which tightens with sciatica.
- Pelvic tilts. Lie on your back with knees bent and feet flat. Gently tighten your abdominal muscles and press your lower back into the floor. Hold for 5 seconds, then relax. This activates your core stabilizers without loading the spine.
- Walking. Simple upright walking is one of the best things you can do. It keeps the spine gently decompressed, encourages circulation to the disks, and activates the muscles that support the lumbar spine. Start with 10 to 15 minutes and build up to 30 minutes daily as pain allows.
Movements to avoid during recovery:
- Forward bending exercises like sit-ups or toe touches
- Heavy leg presses or squats with a load
- Any exercise that makes your leg pain travel further down
- High-impact activities like running or jumping in the acute phase
Recovery framework to follow: Think of your recovery in three phases. Phase one covers the first one to two weeks – focus on pain control through rest, ice, and heat, and very gentle movement. Phase two runs from week two to week six – introduce stretching and daily walking. Phase three begins around week six – gradually work up to core strengthening exercises. Do not rush into phase three before phase two feels comfortable.
Posture and Daily Movement Adjustments
How you hold yourself and move throughout the day has a major impact on how quickly your disk heals. Small adjustments done consistently every single day make a real difference over weeks.
When sitting:
- Choose a firm chair with good lower back support
- Keep your feet flat on the floor and your hips at roughly a 90-degree angle
- Maintain a slight inward curve in your lower back – do not let it round forward
- Place a small rolled towel or lumbar support behind your lower back if needed
When standing:
- Avoid locking your knees or letting your pelvis tilt forward
- Engage your core muscles lightly throughout the day
- If standing for long periods, place one foot on a low step and alternate feet regularly
When lifting – even light items:
- Always bend at the hips and knees, never at the waist
- Keep the object close to your body
- Never twist your spine while holding something – turn your whole body by moving your feet instead
Read: Complete Guide to Spine Strengthening
When to See a Doctor and What to Expect
If your symptoms are gradually improving with self-care, you may not need a doctor right away. However, you should seek medical evaluation if:
- Pain is severe and not improving after two to three weeks of home care
- You have significant weakness or numbness in the leg
- Symptoms are getting worse rather than better
- You experience any loss of bladder or bowel control (seek emergency care immediately)
Your doctor will take a medical history and perform a physical examination that includes:
- Testing your reflexes at the knee and ankle
- Checking muscle strength by assessing how you walk on your heels and toes
- Checking sensation in your leg and foot
- Performing a straight leg raise test – if lifting your leg while lying flat reproduces your leg pain, it is a strong indicator of a disk herniation
If they suspect a significant herniation, an MRI scan will likely be ordered. MRI provides clear images of soft tissue and shows exactly which disk is affected and which nerve roots are involved. A CT scan may be used as an alternative if an MRI is not possible.
Nonsurgical Medical Treatments
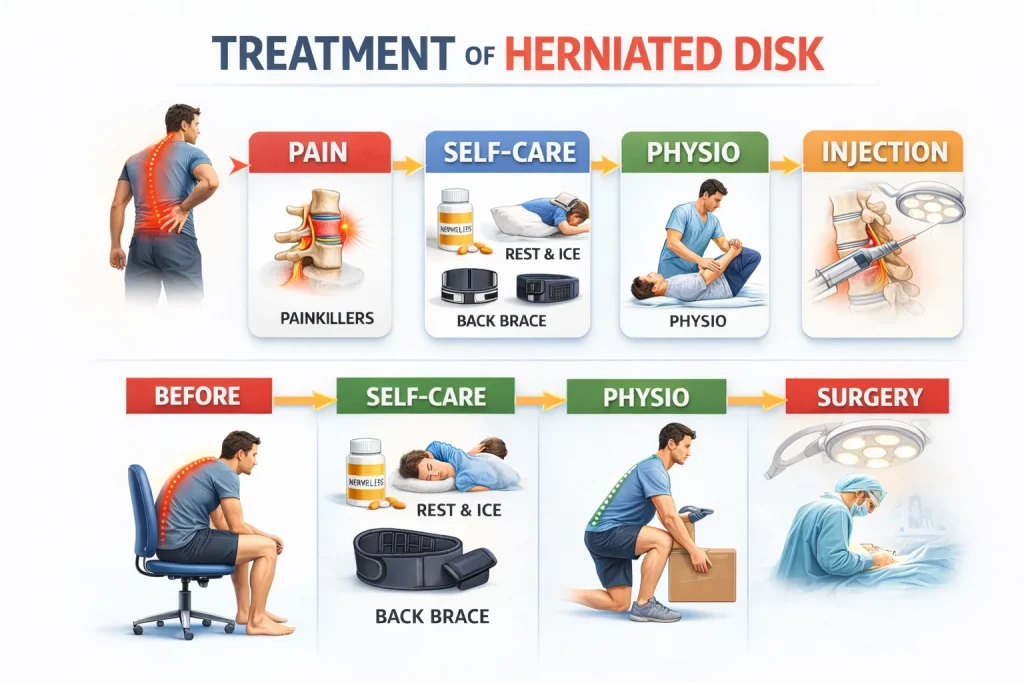
If self-care alone has not provided enough relief, your doctor has several options available:
- Physical therapy – a physiotherapist can design a targeted program addressing the specific muscle imbalances contributing to your pain
- Epidural steroid injection – a cortisone-based medication injected into the space around the affected nerve root can provide meaningful short-term pain relief by reducing inflammation, particularly for people with severe or persistent sciatica
- Prescription medication – in some cases, stronger anti-inflammatory or nerve pain medications may be prescribed for short-term use
These nonsurgical treatments do not repair the disk. They relieve symptoms while your body naturally heals the herniation over time.
Surgery – The Last Resort
Only a small percentage of people with a herniated lumbar disk ever need surgery. Surgery is typically considered when:
- Nonsurgical treatment has not worked after several months
- Muscle weakness is significant and progressively worsening
- Daily function and walking are severely impaired
- Cauda equina syndrome is present (this is a surgical emergency)
The most common procedure is a microdiskectomy, where a surgeon removes the herniated portion of the disk through a small incision using magnification. A newer approach called endoscopic diskectomy uses an even smaller incision with a camera-guided tube, potentially offering faster recovery with less scarring.
Both procedures have generally good outcomes, especially for relieving leg pain. Most patients can resume normal activities after a period of recovery.
Important to know: even after surgery, there is a 20 to 25% lifetime chance of the disk herniating again. This makes the lifestyle habits covered in this article just as important after surgery as before.
How Long Does Recovery Take?
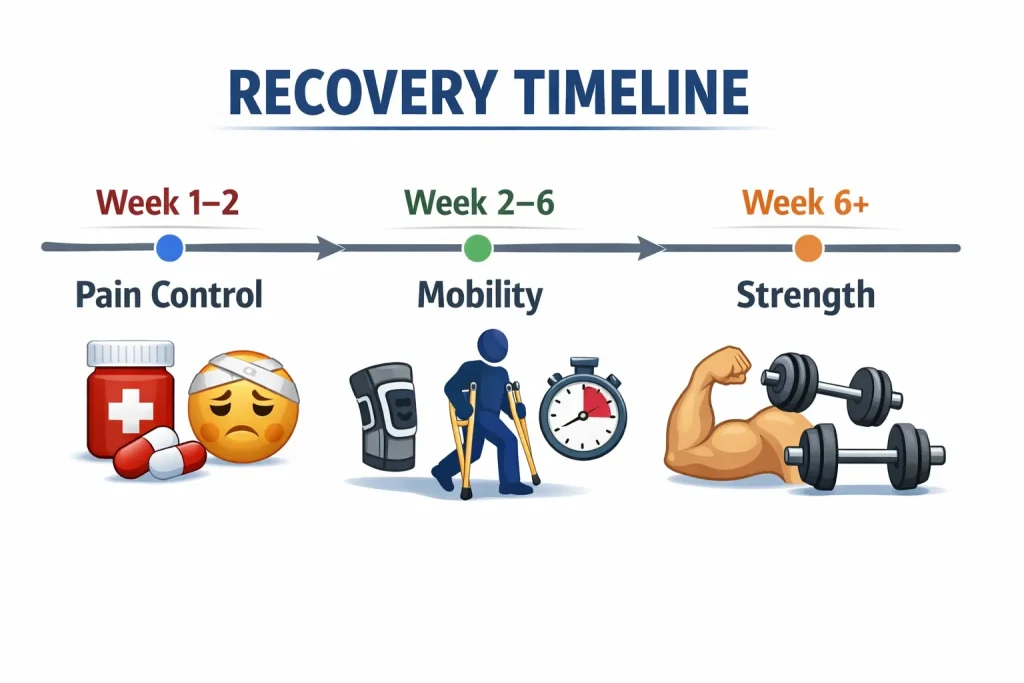
Most people with a herniated disk in the lower back see meaningful improvement within four to six weeks of consistent self-care. The majority are largely symptom-free within three to four months.
Here is the typical progression of recovery:
- Pain is usually the first symptom to improve
- Leg strength returns next as nerve pressure reduces
- Sensation – numbness and tingling – is often the last to fully resolve and may linger even after pain has gone. This is a sign of gradual nerve healing, not a reason for concern.
Recovery is not always a straight line. Flare-ups are common, especially early on. A day where you sit too long, sleep in an awkward position, or overdo physical activity can temporarily worsen your symptoms. This is normal and does not mean you have undone your progress. Focus on the trend over weeks and months, not any individual bad day.
Preventing a Herniated Disk From Coming Back
Because recurrence rates are significant – up to one in four people experience another herniation over their lifetime – taking prevention seriously after recovery is genuinely worthwhile.
Key prevention habits to build into your daily life:
- Strengthen your core consistently. The muscles of your abdomen and lower back form a natural protective corset around your lumbar spine. Exercises like dead bugs, bird dogs, side planks, and glute bridges are particularly effective and spine-friendly. Even 10 to 15 minutes a day makes a measurable difference.
- Maintain a healthy weight. Even modest weight loss reduces the mechanical stress on your lumbar disks significantly over time. This is one of the highest-impact long-term changes you can make for spinal health.
- Stay physically active. Regular moderate exercise – walking, swimming, cycling, yoga – keeps the muscles around your spine engaged, maintains healthy blood flow to your disks, and supports a healthy weight. Inactivity is one of the most underrated risk factors for disk herniation and recurrence.
- Practice good lifting mechanics every day. Good technique is not just for gym sessions – it applies every time you pick up a child, unload groceries, or grab something from a low shelf. The cumulative protective effect of consistent body mechanics over the years is significant.
- Break up prolonged sitting. If you sit for work, take a movement break every 30 to 45 minutes. Stand up, walk briefly, and reset your posture. Investing in a supportive chair with good lumbar support is worthwhile if you sit for most of the day.
- Do not smoke. If you smoke and care about your back, quitting is one of the most protective steps you can take. The connection between smoking, reduced disk oxygenation, and accelerated degeneration is well established.
Conclusion
A herniated disk in the lower back is painful and disruptive – but it is also one of the most manageable spine conditions there is. The vast majority of people recover fully without surgery, and much of that recovery is driven by what you do for yourself at home.
Key takeaways from this guide:
- A herniated disk occurs when the gel-like center of a spinal disk pushes through its outer wall and irritates nearby nerves
- Age-related disk degeneration is the most common cause, accelerated by poor lifting habits, prolonged sitting, excess weight, inactivity, and smoking
- Lower back pain and sciatica are the most common symptoms; loss of bladder or bowel control requires immediate emergency care
- Most cases resolve within three to four months with consistent self-care, including smart rest, ice and heat, anti-inflammatories, gentle exercise, and posture awareness
- Surgery is a last resort needed by only a small minority of patients
- Building a strong core, staying active, and practicing good daily mechanics are the best defenses against recurrence
You have more control over this condition than you might think. Start with one small change today, and build from there.
FAQs
Can a herniated disk in the lower back heal on its own?
Yes, in many cases it can. The herniated gel material is often gradually reabsorbed by the body over time. Most people see significant improvement within three to four months. Self-care practices like rest, movement, and posture adjustments meaningfully support and accelerate this natural healing process.
What is the difference between a herniated disk and a bulging disk?
A bulging disk means the outer ring has pushed outward but remains intact. A herniated disk is more severe – the inner gel has actually broken through the outer ring. Both can cause pain if they press on nerves, but a herniated disk tends to produce more intense symptoms because of added chemical irritation from the exposed nucleus material.
How long should I try self-care before seeing a doctor?
Most guidelines suggest trying conservative self-care for two to four weeks before seeking medical evaluation, provided symptoms are improving. If pain is severe from the outset, if you notice significant leg weakness or worsening symptoms, or if you experience any loss of bladder or bowel function, seek medical attention immediately without waiting.
What is sciatica, and how does it relate to a herniated disk?
Sciatica is pain that travels along the path of the sciatic nerve – from the lower back through the buttock and down the back of the leg. It is one of the most characteristic symptoms of a herniated lumbar disk. When the herniated disk presses on the sciatic nerve root, it creates the distinctive shooting or burning sensation most people associate with sciatica.
Is it safe to exercise with a herniated disk?
Yes – appropriate exercise is actually an important part of recovery. Gentle walking, pelvic tilts, knee-to-chest stretches, and water-based exercise are generally well-tolerated and beneficial. Avoid forward-bending exercises, heavy lifting, and anything that worsens your leg symptoms. Working with a physical therapist to develop a tailored program is the safest approach if you are unsure where to start.
What are the chances of a herniated disk coming back after recovery?
Studies estimate that up to 20 to 25% of people experience another disk herniation over their lifetime, whether treated surgically or nonsurgically. Building core strength, maintaining a healthy weight, staying active, and consistently practicing good posture and lifting mechanics are the best protections against recurrence.