Key Takeaways:
- A muscle cramp is a sudden, painful tightening of a muscle that you cannot control, and it can happen to anyone at any time.
- The most common causes are dehydration, low levels of minerals such as magnesium and potassium, and muscles becoming too tired from exercise.
- To get quick relief, stop moving, gently stretch the cramped muscle, massage it, and drink water or an electrolyte-rich drink immediately.
- You can prevent most cramps by stretching regularly, staying well hydrated, eating mineral-rich foods, and building up your fitness level slowly.
- See a doctor if cramps happen often without any clear reason, spread across your whole body, or come with numbness, weakness, or leg pain while walking.
It hits without warning. You are deep in sleep, mid-run, or simply stretching in the morning – and suddenly your calf locks up in a fierce, unrelenting spasm. A muscle cramp is one of the most common musculoskeletal complaints, yet most people dismiss it without a second thought.
But for athletes, older adults, and people with nutritional deficiencies, frequent muscle cramps often signal something your body urgently needs you to address.
This guide covers everything you need to know: what muscle cramps are, why they happen, which muscles are most affected, how to treat them at home, and when to stop self-treating and see a specialist.
What is a Muscle Cramp?
A muscle cramp is a sudden, involuntary contraction of a muscle that does not relax on its own. The muscle fibers seize up and refuse to release, causing sharp, intense pain that can last anywhere from a few seconds to 15 minutes or more.
You may have heard muscle cramps called by other names:
- Charley horse – a painful cramp, usually in the calf or thigh
- Muscle catch – a sudden, localized spasm felt during movement
- Muscle lock – when the muscle feels completely frozen
- Muscle spasm – a broader term that includes both cramps and involuntary twitches
Spasm vs Cramp: A spasm is any involuntary muscle contraction. A cramp is a specific, painful, sustained type of spasm. All cramps are spasms – but not all spasms are cramps.
Muscle cramps can affect part of a muscle, a whole muscle, or an entire group of muscles working together. They are painful, often visible under the skin, and can recur multiple times before fully resolving.
Which Muscles Are Most Commonly Affected?
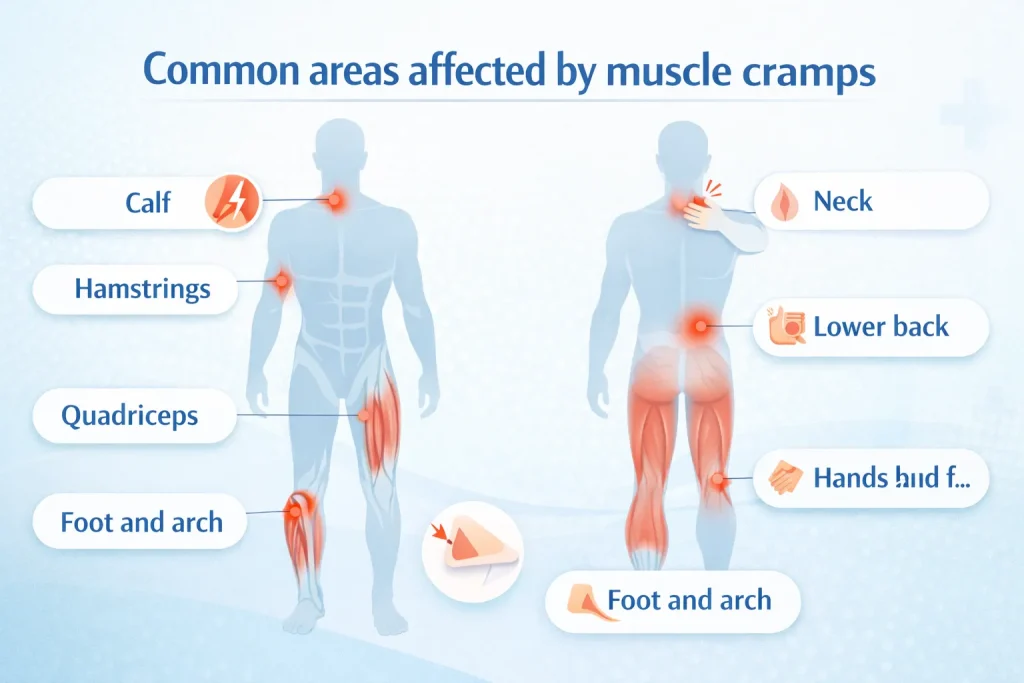
Cramps can affect any skeletal muscle in the body. The most frequently reported areas include:
- Calf muscles (gastrocnemius) – the classic calf cramp or charley horse
- Hamstrings – back of the thigh, common during or after exercise
- Quadriceps – front of the thigh, often seen in runners and cyclists
- Foot and arch muscles – foot cramps at night are a classic sign of electrolyte depletion
- Hands and fingers – cramps in fingers and toes after repetitive tasks
- Inner thigh – inner thigh cramps are common in swimmers
- Abdomen – stomach muscle cramps during intense core training
- Chest and rib cage – less common but intensely painful
- Neck muscles – neck muscle cramp causes often involve poor posture
- Lower back – lower back spasm symptoms include stiffness and referred pain
Ankle cramps, hip muscle cramps, and arm cramps are also reported regularly, particularly among older adults and post-surgical patients.
What Causes Muscle Cramps?
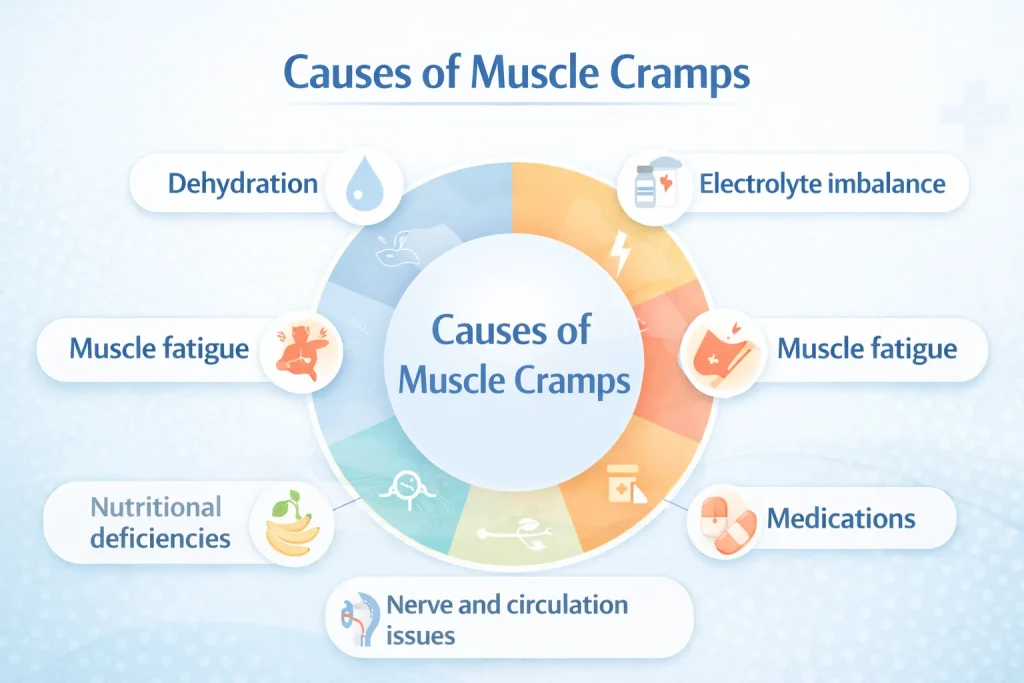
The exact cause of muscle cramps is classified as idiopathic – meaning no single confirmed mechanism exists. However, research strongly supports several contributing factors.
1. Inadequate Stretching and Muscle Fatigue
When muscles are not conditioned for a task, they fatigue faster. An overexerted muscle depletes its oxygen supply and builds up waste products – particularly lactic acid. This triggers a spasm response from the spinal cord, and the muscle keeps contracting even when you want it to stop.
This explains why muscle cramps after a workout are so common, especially lactic acid muscle cramps during heavy resistance or endurance training. Poor conditioning means muscles lack the fiber length and neural efficiency to sustain prolonged effort.
2. Dehydration and Electrolyte Depletion

This is one of the most well-documented reasons for leg cramps. When you sweat – especially in hot weather or during intense exercise – you lose sodium, potassium, magnesium, and calcium. These electrolytes are what your muscles need to contract and relax properly.
Can dehydration cause muscle cramps? Yes. The evidence is clear. Cramps due to dehydration are especially common in:
- Athletes exercising in hot or humid conditions
- Manual workers exposed to high heat
- People who do not hydrate adequately during physical activity
Key insight: It is not just water loss that causes cramps – it is electrolyte loss. Drinking plain water without replenishing minerals can actually dilute remaining electrolytes and worsen cramp risk.
3. Nutritional Deficiencies
What deficiency causes muscle cramps? The most commonly implicated nutrients are:
- Magnesium – essential for muscle relaxation; low magnesium keeps muscles contracted
- Potassium – low potassium disrupts the electrical signals controlling muscle movement
- Calcium – regulates neurotransmitter release that triggers contractions
- Vitamin D – supports calcium absorption; deficiency is widespread in India
- Sodium – lost heavily through sweat; low sodium can trigger cramps all over the body
Muscle cramps deficiency is a real and correctable cause. If you experience what causes severe muscle cramps all over the body with no clear physical trigger, a nutritional panel from your doctor can be very revealing.
4. Age-Related Muscle Loss
Older people are more susceptible to muscle cramps because of natural muscle atrophy that begins in the mid-40s. As muscle mass and strength decline, muscles fatigue more quickly and have a lower threshold for spasm. The body’s thirst response also weakens with age, making dehydration more likely without the person realizing it.
This is why leg cramps in the morning and muscle cramps while sleeping are particularly common in people over 60.
5. Medications
Certain medications are known to increase cramp frequency:
- Diuretics – increase electrolyte loss through urine
- Statins (used for high cholesterol) – can cause painful muscle spasms as a side effect
- Pseudoephedrine (decongestants) – affects neuromuscular function
If you suspect your medication is causing cramps, discuss alternatives with your physician before making any changes.
6. Nerve and Circulation Problems
Not all cramps are caused by the muscle itself. Neurological disorders that cause muscle cramps include:
- Spinal nerve compression (radiculopathy) – pressing on nerve roots causes nerve cramps in the legs
- Peripheral artery disease (atherosclerosis) – reduced blood flow to muscles, especially the calf
- Spinal stenosis – narrowing of the spinal canal that compresses nerves serving the legs
Leg spasms or sudden leg cramps that consistently occur with walking and stop with rest can indicate vascular claudication – a sign of arterial narrowing that requires medical evaluation, not home remedies.
Who is at Greatest Risk for Muscle Cramps?
Some people get muscle cramps far more often than others. Those at elevated risk include:
- Endurance athletes (marathon runners, triathletes, cyclists) – frequent muscle cramps from prolonged effort
- Adults over 65 – due to muscle atrophy, reduced hydration awareness, and medication use
- Pregnant women – hormonal changes and increased metabolic demand affect electrolyte balance
- Overweight or ill individuals – body systems are under greater strain
- Manual laborers working in heat – lose electrolytes rapidly through sweat
- People with chronic conditions – kidney disease, thyroid disease, liver cirrhosis, and ALS can all cause frequent muscle cramps
Athletes are also more likely to experience cramps in the preseason when the body is poorly conditioned, and cramps often develop near the end of intense exercise or 4 to 6 hours afterward.
Muscle Cramps Symptoms: What Do They Feel Like?
How do cramps feel? Anyone who has had one knows – but here is a clinical breakdown:
- Sudden, sharp, involuntary tightening of the muscle
- Intensity ranges from a mild twitch to agonizing, immobilizing pain
- The muscle may feel rock-hard to the touch
- Visible distortion or rippling under the skin is common
- A single cramp can last from a few seconds to over 15 minutes
- It may recur multiple times before fully resolving
- Residual soreness or tenderness often follows for hours
Charley horse symptoms include intense tightening in the back of the lower leg, muscle hardness, involuntary toe-pointing, and difficulty walking immediately after.
Severe muscle cramps – especially those involving multiple muscle groups or spreading across the whole body – should always prompt a medical evaluation.
Home Remedies for Muscle Cramps: How to Get Relief Fast

The good news: most muscle cramps resolve on their own. Here is how to treat them effectively at home.
Step 1 – Stop the Activity
The moment a cramp strikes, stop whatever triggered it. Continuing to push through a muscle lock risks injury.
Step 2 – Stretch and Massage
Gentle stretching is the most effective immediate intervention. Extend the muscle in the direction opposite to the cramp and hold the position. For a calf cramp, flex your foot upward. For a hamstring spasm, straighten the leg. Massage the muscle with firm, circular pressure at the same time – this mechanically interrupts the spasm cycle.
Step 3 – Apply Heat or Cold
- Heat (warm compress or hot water bottle) – best for tense, knotted muscles
- Cold (ice pack wrapped in cloth) – better for sore or inflamed muscles after the cramp passes
Do not apply ice directly to skin. Use a cold pack for 15–20 minutes at a time.
Step 4 – Rehydrate and Replenish Electrolytes
Drink water immediately, then follow up with:
- Low-sugar sports drinks (contain sodium and potassium)
- Coconut water – a natural source of potassium and magnesium
- Low-fat cow’s milk – provides calcium, potassium, and protein
- Electrolyte-rich foods: bananas, spinach, lentils, yogurt, sweet potato
A muscle cramp relief spray containing magnesium or menthol can also provide quick topical relief for surface-level spasms.
Medicine for Muscle Cramps
Over-the-counter options include:
- Magnesium supplements – particularly useful for nighttime cramps or deficiency-related cramps
- Electrolyte tablets – for rapid replenishment after intense exercise
- Topical analgesics – sprays or gels with menthol or camphor for localized pain
The best medicine for muscle cramps depends on the underlying cause. Do not self-prescribe drugs for muscle cramps – particularly muscle relaxants – without a physician’s evaluation. For recurrent or severe cramps, your doctor should assess for nerve involvement, circulation issues, or mineral deficiencies first.
When to See a Doctor: Seek medical care if cramps are severe, happen frequently without a clear cause, do not respond to home treatment, or come with numbness, weakness, or swelling in the limb.
How to Prevent Muscle Cramps: 7 Evidence-Based Strategies

Prevention is always more effective than treatment. Here is how to avoid muscle cramps:
1. Build a Consistent Stretching Routine
Do flexibility exercises before and after every workout, targeting the muscle groups most prone to cramping – calves, hamstrings, and quadriceps. Always warm up before stretching. A brisk 5-minute walk or light jog prepares muscles for deeper flexibility work.
2. Stretch the Three Key Muscle Groups
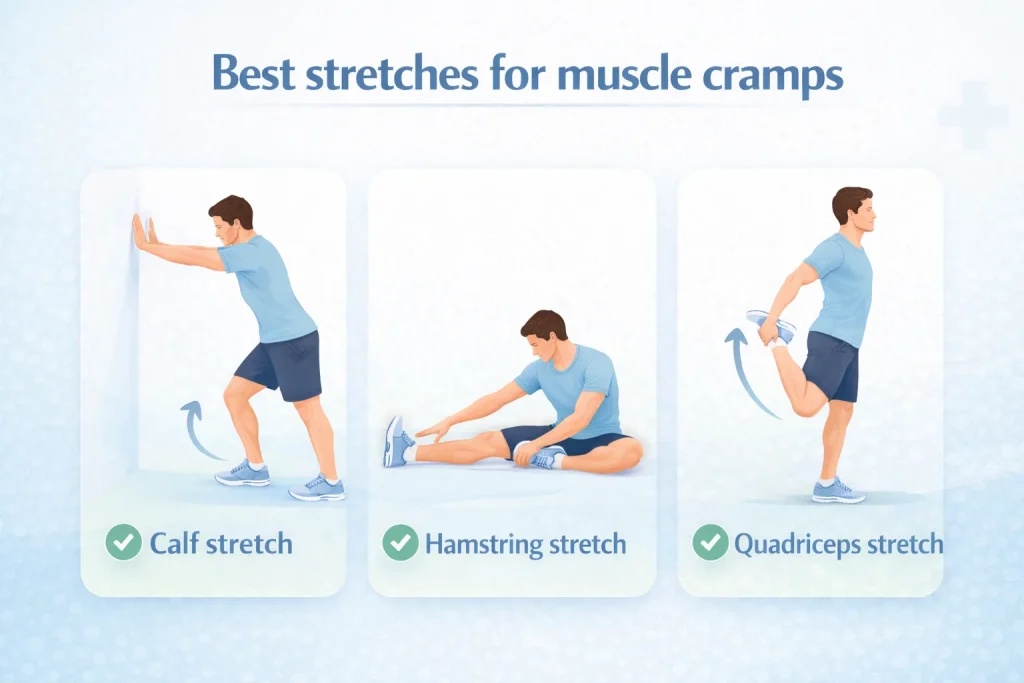
Calf Muscle Stretch: Lean forward against a wall, one foot in front of the other, back leg straight with heel flat on the floor. Hold 15–30 seconds.
Hamstring Muscle Stretch: Sit tall with legs extended straight in front. Slide your palms toward your ankles, keeping your back long and chest open. Hold 30 seconds.
Quadriceps Muscle Stretch: Stand near a wall for balance. Bring one heel toward your buttock, grasp the ankle, and hold for 30 seconds. Keep knees together throughout.
These three stretches – done daily – are among the most effective tools for preventing muscle cramps, especially thigh and leg cramps.
3. Hydrate Before, During, and After Exercise
Do not wait until you are thirsty. By the time thirst kicks in, you may already be mildly dehydrated. Increase water intake in hot weather and replenish electrolytes after any long or intense activity.
4. Improve Overall Fitness Gradually
Cramps are far more likely when your body is poorly conditioned. Increase exercise intensity by no more than 10% per week. This is especially important for athletes in preseason training and for those returning to exercise after illness or orthopaedic recovery.
5. Correct Nutritional Deficiencies
Get a blood test to check magnesium, potassium, calcium, vitamin D, and sodium levels if you experience frequent muscle cramps. Work with a physician or dietitian to correct any deficiencies through diet or supplementation.
6. Manage Medications Carefully
If you are taking diuretics, statins, or other medications known to trigger cramps, speak with your doctor about dose timing, electrolyte monitoring, or alternative options.
7. Adjust Your Sleep Habits
For people who get muscle cramps while sleeping:
- Keep bedsheets loose around the feet
- Avoid sleeping with feet in a pointed (plantar-flexed) position
- Do a brief calf and foot stretch before bed each night
Special Situations: Cramps You Should Not Ignore
Cramps After Exercise
Muscle cramps after a workout that persist for hours may indicate more than simple fatigue. Sustained post-exercise cramps can signal severe electrolyte loss, rhabdomyolysis (muscle breakdown), or an underlying metabolic issue. If they occur alongside dark urine or muscle weakness, seek emergency care immediately.
Cramps While Sleeping
Muscle cramps while sleeping – especially in the calf and foot – are very common in adults over 50. Foot cramps at night, a classic sign of low potassium or magnesium, should be evaluated if they regularly disrupt sleep.
Cramps All Over the Body
What causes severe muscle cramps all over the body? This pattern is more concerning than localized cramps. Possible causes include severe dehydration, kidney dysfunction, thyroid disorders, or a serious neurological condition. Body cramps that are widespread and unprovoked require prompt medical attention – not home remedies.
Leg Cramps with Pain While Walking
Sudden leg cramps during walking that are relieved by rest can point to peripheral artery disease. Calf pain in one leg that appears with exertion and disappears at rest is a hallmark of vascular claudication – a condition that requires vascular investigation, not stretching.
When to See a Doctor for Muscle Cramps

The vast majority of cramps are harmless and resolve on their own. But muscle cramps can sometimes be a sign of a more serious health condition. See an orthopaedic or general physician if:
- Cramps are severe, frequent, or progressively worsening
- They happen consistently without obvious physical causes like exercise or dehydration
- Home remedies provide no relief
- You have other symptoms: numbness, tingling, weakness, swelling, or skin changes in the affected limb
- You suspect a nerve cramps pattern – nerve cramps in legs are often deeper, burning, and linked to back problems
- Your medication may be causing the cramps
- You have a history of liver, kidney, thyroid, or vascular disease
Your doctor may investigate for radiculopathy, spinal stenosis, atherosclerosis, thyroid dysfunction, cirrhosis, chronic infection, or – in rare cases – ALS. Early diagnosis is always better than delayed treatment.
Muscle Cramps in Hindi: Common Terms Patients Use
For patients more comfortable with regional terminology:
- Muscle cramps meaning in Hindi: मांसपेशियों में ऐंठन (Maansapeshiyon mein ainthan)
- Bainta in English: Bainta = cramp or spasm, commonly used in North Indian dialects
- Cramps in Marathi: पेटके (Petke)
- Muscle catch meaning: A colloquial term for a sudden localized spasm – equivalent to “muscle catch in legs.”
Understanding these terms helps patients communicate their symptoms more precisely to their healthcare provider.
Conclusion
Muscle cramps are common – but they should not be accepted as inevitable. Most cramps respond well to stretching, hydration, and electrolyte management. However, frequent, severe, or unexplained cramps often signal something deeper: a nutritional deficiency, nerve compression, vascular insufficiency, or an underlying systemic condition.
The key takeaways from this guide:
- Understand your cramp pattern – when, where, and how often they occur
- Treat immediately with stretching, massage, heat or cold, and rehydration
- Prevent proactively through fitness conditioning, targeted stretching, and correct nutrition
- Never ignore cramps that are severe, recurrent, or spread across the whole body – get a proper evaluation
At Deformity, our clinical team approaches every musculoskeletal complaint with precision and compassion. If muscle cramps are affecting your sleep, your training, or your daily life – you deserve expert guidance, not guesswork.
Visit deformity.co.in to consult with our orthopaedic specialists and take the first step toward lasting relief.
FAQs
What is a muscle cramp?
A muscle cramp is a sudden, involuntary, painful contraction of a skeletal muscle. It can affect one muscle or a group, lasting seconds to minutes, and is most common in the legs and feet.
What causes muscle cramps?
Common causes include dehydration, electrolyte depletion (potassium, magnesium, calcium), muscle fatigue, poor conditioning, medication side effects, nerve compression, and age-related muscle loss.
How to stop muscle cramps fast?
Stop the triggering activity, gently stretch and massage the cramping muscle, apply heat or cold as appropriate, and rehydrate with water or an electrolyte drink. Most cramps resolve within 15 minutes with these steps.
Can dehydration cause muscle cramps?
Yes. Dehydration reduces blood volume and depletes electrolytes like sodium and potassium, both essential for normal muscle contraction and relaxation. Cramps due to dehydration are very common during exercise.
What deficiency causes muscle cramps?
Magnesium, potassium, calcium, sodium, and vitamin D deficiencies are all linked to frequent muscle cramps. A simple blood test from your doctor can identify which nutrient you are lacking.
Why do muscle cramps occur at night?
Nocturnal muscle cramps in the calf and foot may result from sleeping in a position that shortens the muscle, electrolyte shifts during sleep, reduced circulation, or low magnesium and potassium levels.
What is the difference between a spasm and a cramp?
A spasm is any involuntary muscle contraction. A cramp is a specific, painful, sustained type of spasm. All cramps are spasms, but not all spasms qualify as cramps. Cramps are generally more intense and longer-lasting.
When to worry about leg cramps?
See a doctor if cramps are frequent, severe, unresponsive to home treatment, or associated with leg weakness, numbness, or consistent pain during walking that stops with rest.
What are the best home remedies for muscle cramps?
Stretching, massage, heat or cold application, hydration, and electrolyte replenishment are the most effective home remedies. Magnesium-rich foods like bananas, spinach, and lentils also help with prevention.
Do neurological disorders cause muscle cramps?
Yes. Neurological disorders that cause muscle cramps include spinal stenosis, nerve root compression (radiculopathy), peripheral neuropathy, and ALS. Persistent or unexplained cramps should be evaluated by a specialist.